
This month is “Stoptober”, the annual campaign encouraging smokers to stop smoking for 28 days during the month of October. It’s an opportunity I heartily recommend people take, if they wish: choosing to stop smoking for 28 days gives you an increased chance of stopping smoking for good, like I did, a decade or so ago. And that would be a good thing, for all sorts of reasons.
On 1st October, South London and Maudsley NHS Trust (SLaM) went “smoke free”. This means that, across its entire site, no-one – staff, patient, visitor – will be permitted to smoke. The ban covers all of its hospital sites, namely the Maudsley Hospital in Southwark, Lambeth Hospital, Bethlem Royal Hospital in Bromley and the Ladywell Unit at Lewisham Hospital. SLaM, whether on ward or – and this is new – outdoors. And here’s the issue I’m highlighting today: that includes a ban on detained patients who do not have leave smoking. People struggling to cope with a mental health crisis and sectioned will now have have no opportunity to go and have a cigarette designated outdoor areas in the grounds, the ‘garden’ of their temporary surrogate home.
I mention SLaM simply because they are one of the only NHS trusts to introduce a total ban and because I’ve chatted with them on twitter about their policy. It’s funny what I randomly stumble across on twitter.
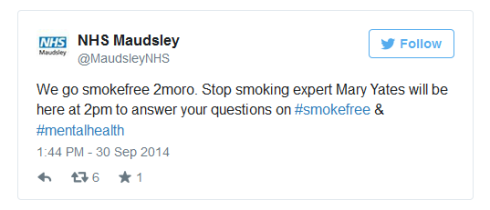
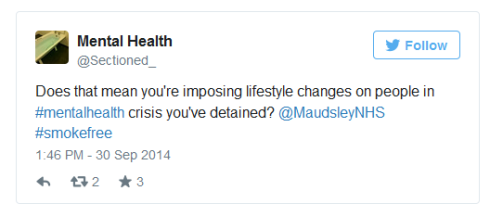
I asked SLaM whether it would be requiring staff to be ‘smoke free’ 24 hours a day; or whether detained patients would be permitted to smoke outside of office hours; after all, if a policy is about health, and both staff and patients have the lungs, the same policy should apply.
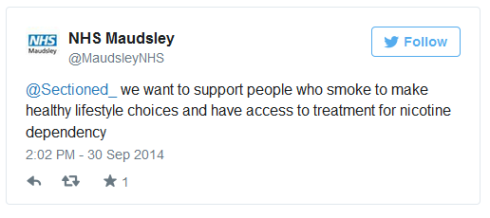
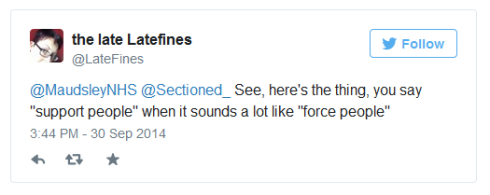
“[S]upport[ing] people who smoke to make healthy lifestyle choces and have access to treatment for nicotene dependency” is something I encourage and does not depend on imposing a total ban. However, while staff were to be encouraged to stop smoking, patients were to be forced to do so. I asked whether, to help make wards healthier, would detained patients have access to exercise, healthy food, fresh air? Would harmful practices like forced medication be banned. No response.

Extending the ban on smoking on NHS premises is NHS policy. The National Institute for Health and Care Excellence (NICE) issued new guidelines last year, updating those from 2008 which banned smoking indoors. SLaM matron Mary Yates contributed to the development of NICE’s national smokefree guidelines which is perhaps why SLaM is one of the early adopters. But what of psychiataric detainees? Somehow, along the way, the rights of mental health patients to make choices about our own lives seem to have been bulldozed by the familiar patronising undertones that infect the whole of mental health services.
“But smoking is harmful! We have a duty to our patients! We must do everything we can to encourage and support patients to make healthy lifestyle choices!” I agree with all of that. However, smoking is not a medical or mental health emergency: it is a bad habit, an unhealthy habit, a poor lifestyle choice, one to be discouraged – and one where people need every opportunity and support to stop or cut down if they choose. Patients with mental health problems die decades before the general population from conditions such as lung cancer, heart disease and stroke. It’s a serious problem and one which needs to be addressed, urgently, diligently and intensely.
However, no one is sectioned for nicotine addiction. No one is in immediate danger of death from being a cigarette smoker. Being a smoker is not a medical emergency. The presenting problem is a mental health crisis. A mental health crisis is not the time to impose lifestyle changes. To seek to impose lifestyle changes at that time is, as Mark Brown put it, “awesome mission creep”.
What is the reason for extending the ban on smoking into the grounds of psychiatric hospitals? The indoors ban introduced a decade ago had clear aims, but what are the aims of the outdoor ban? SLaM says in its page on it’s new ‘smoke free’ policy that its aims are “[t]o create a healthier environment for everyone] and to “reduce … inequality”. Are those aims – vague as they seem – achieved by imposing temporary abstinence on psychiatric detainees? Is there evidence that enforced temporary abstinence provides sustained behaviour change?

For instance, do detainees prevented from smoking whilst on ward remain abstinent on discharge – or, say, 6 months post-discharge? We don’t know because, as the NICE guidelines acknowldge, there are huge gaps in the evidence. This is an evidence-free zone. It is a policy based on a toxic combination of public health moralising about smoking and paternalism about people with mental health problems.
And it is a dangerous policy too. Not only is there no evidence that enforced temporary abstinence improves health outcomes post-discharge, there is clear evidence that, in the short-term, bans are potentially dangerous for patients. This is because smoking impacts on the levels of medication patients require. Most inpatient stays are short-term – two to three weeks on average – and, for a short-term stay, stopping smoking suddenly can mean a dangerous rise in in the levels of medication in the bloodstream that will need to be monitored (which does not happen). And, on discharge, any levels of medication established during detention will be impacted on the (likely) resumption of smoking on release.
Smoking is just about the worst thing anyone can do to their body apart from, say, sticking their head into a giant mincer & pressing the on-button. I am a non-smoker and wish everyoe else was too. I wish smoking had never been invented. It breaks my heart when friends smoke (and makes me turn up my nose and back away from the smell); I want them to be around, not die prematurely early from smoking-related disease. That’s why I want all the help in the world made available to people with mental health problems who wish to stop smoking. But I don’t for one second think that unevidenced temporary enforced abstinence should be any part of the solution. There’s a difference between saying “Smoking is harmful” (which clearly it is, and has a disproportionately large impact on people with mental health problems) and saying “This new policy is the most best & effective way to reduce that harm” – which clearly it isn’t, because there’s no evidence base.
.
 Background information:
Background information:
.
Storify stories
.
Blogosphere
.
Input from patients:
- Here I’ll put links to all the patient consultations I come across *taps fingers* *checks watch* *waits*
Tags: coercion, discrimination, Mental health, NHS, prejudice, psychiatric wards












